What is a neck hernia?
A bulging intervertebral disc
A neck hernia is a bulge in an intervertebral cervical disc. This bulge presses on a nerve attached to an arm, thus possibly causing pain radiating down a shoulder or arm. Other symptoms may include tingling in the patient’s hand or fingers, and occasionally a loss of strength. If the latter occurs, an arm nerve will have stopped functioning. Generally speaking, symptoms will present in either the left arm or the right arm (not both).
The cervical spine has 7 vertebrae, with intervertebral discs between them. These discs serve as shock absorbers, so to speak, and they increase the spine’s elasticity. Along with the neck muscles, they allow the neck to move.
The spinal canal houses the spinal cord. Arm nerves branch off the spinal cord on both the left- and right-hand sides of the spine, very close to intervertebral discs. The most common type of neck hernia is located between the sixth and seventh cervical vertebrae, but hernias also occur between other vertebrae.
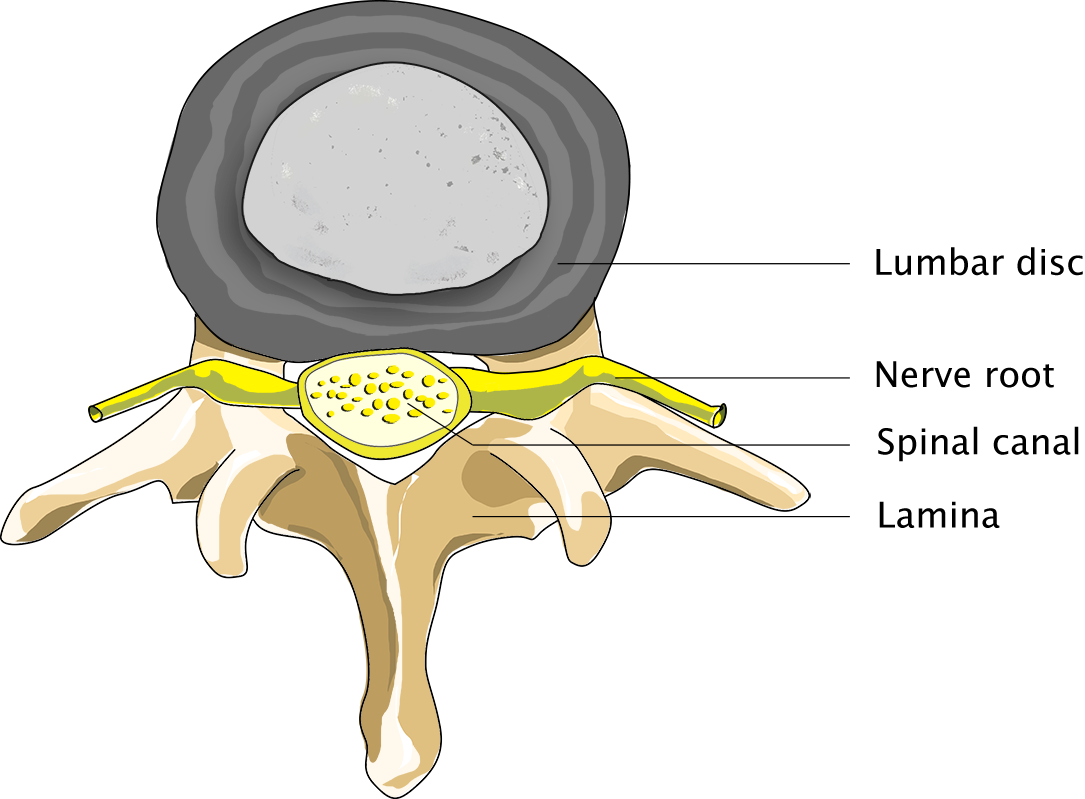
Normal person
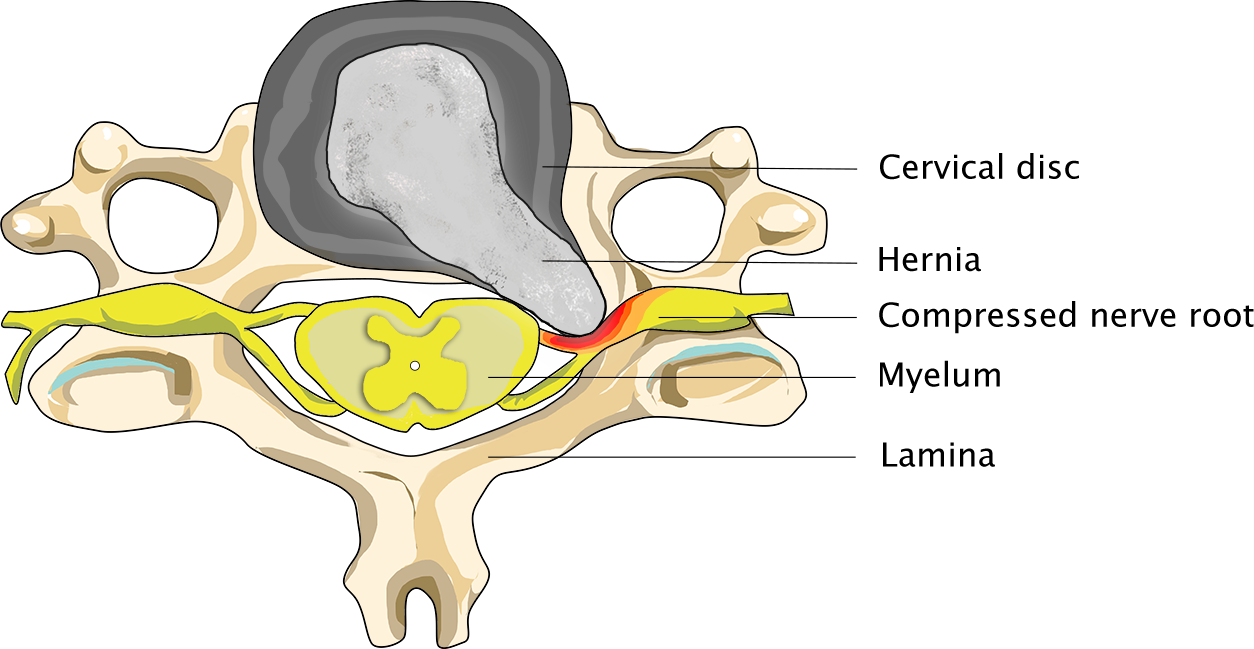
Person suffering from a neck hernia
In this article
Use the overview below to read more about a specific topic:
Causes of a neck hernia
Degeneration of an intervertebral disc
Degeneration of an intervertebral disc is a normal process that happens to everyone, although some people will be affected more severely than others. However, a disc may also suffer a tear in its outer ring, through which the contents of the disc may be forced outwards, towards the spinal canal. Generally, the ring will tear in its weakest spot, which is the spot where an arm nerve branches off the spinal canal.
Unknown cause
Anyone can suffer a hernia, and we do not know why some people are affected while others are not. However, it is known that some families are more prone to hernias than others. It is also known that smoking negatively affects the quality of the vertebrae and of the intervertebral discs.
Symptoms of a neck hernia
Pain radiating down an arm
Patients often suffer neck pain before the onset of a neck hernia. Neck hernia symptoms include pain radiating down an arm, possibly accompanied by numbness or tingling. These symptoms will present more or less in the service area of the nerve that is being pressed upon, although this is not as obvious with neck hernias as it is with low-back hernias. The pressure exerted on the nerve may cause nerve function loss.
Loss of strength in one or more muscles
Nerves serve a dual function: they serve the muscles, but also an area of skin. In other words, each nerve comes with its own muscle and area of skin. Neck hernia patients may suffer a loss of strength in one or more muscles, and may or may not experience tingling or numbness. Since coughing, sneezing or straining causes the pressure in the spinal canal, and therefore the pressure exerted on the arm nerves, to increase, the pain radiating down the arm may become more intense while a patient is coughing or sneezing.
If a patient suffers a larger hernia located towards the middle of the spine (possibly near an already constricted spinal canal), a great deal of pressure may be exerted on the spinal cord, which may result in a loss of strength and/or sensation disorders in the legs, in addition to the arm and neck pain already present. This, in turn, may result in a changed gait.
Diagnosis of a neck hernia
Neurological examination
First of all, a neurologist will listen to your symptoms. After that, s/he will carry out a thorough neurological examination. An additional examination will have to be carried out to determine whether the pain in the arm is indeed caused by a bulging intervertebral disc.
Sometimes X-ray images will have been taken by this stage. Such images do a great job of showing the patient’s bone structure, i.e., the vertebrae. This provides an insight into the shape of the cervical vertebrae and how the vertebrae are positioned in relation to each other. For their part, MRI scans are performed to show the ‘soft parts’ of the neck, i.e. the intervertebral discs, muscles and blood vessels.
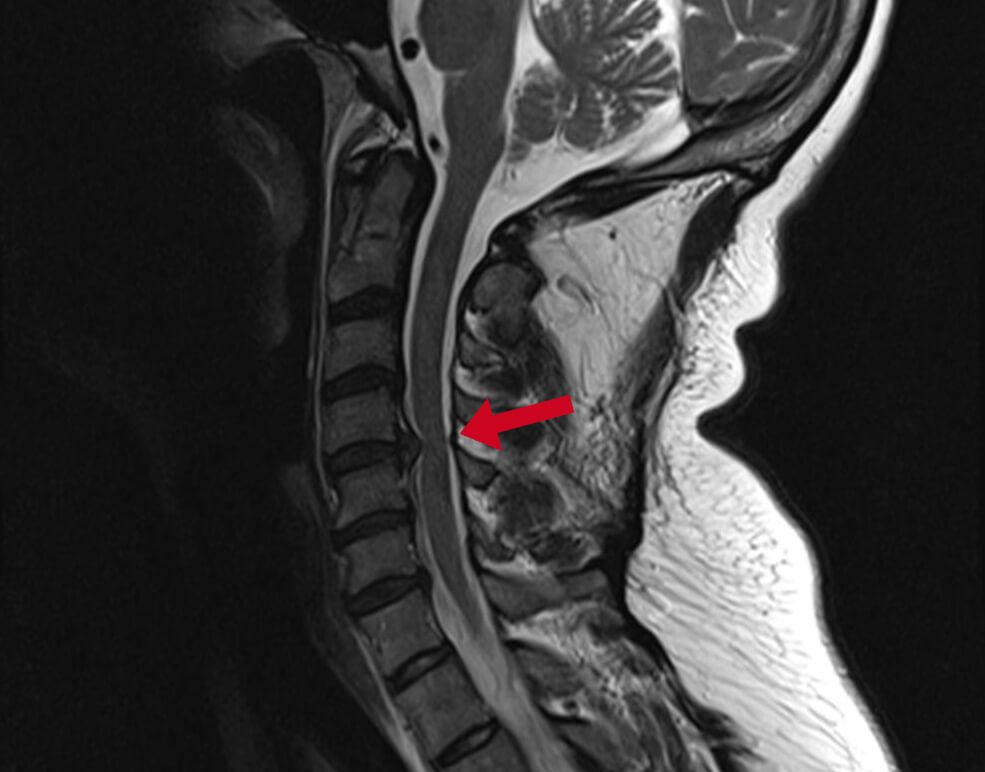
Diagnosis of a neck hernia
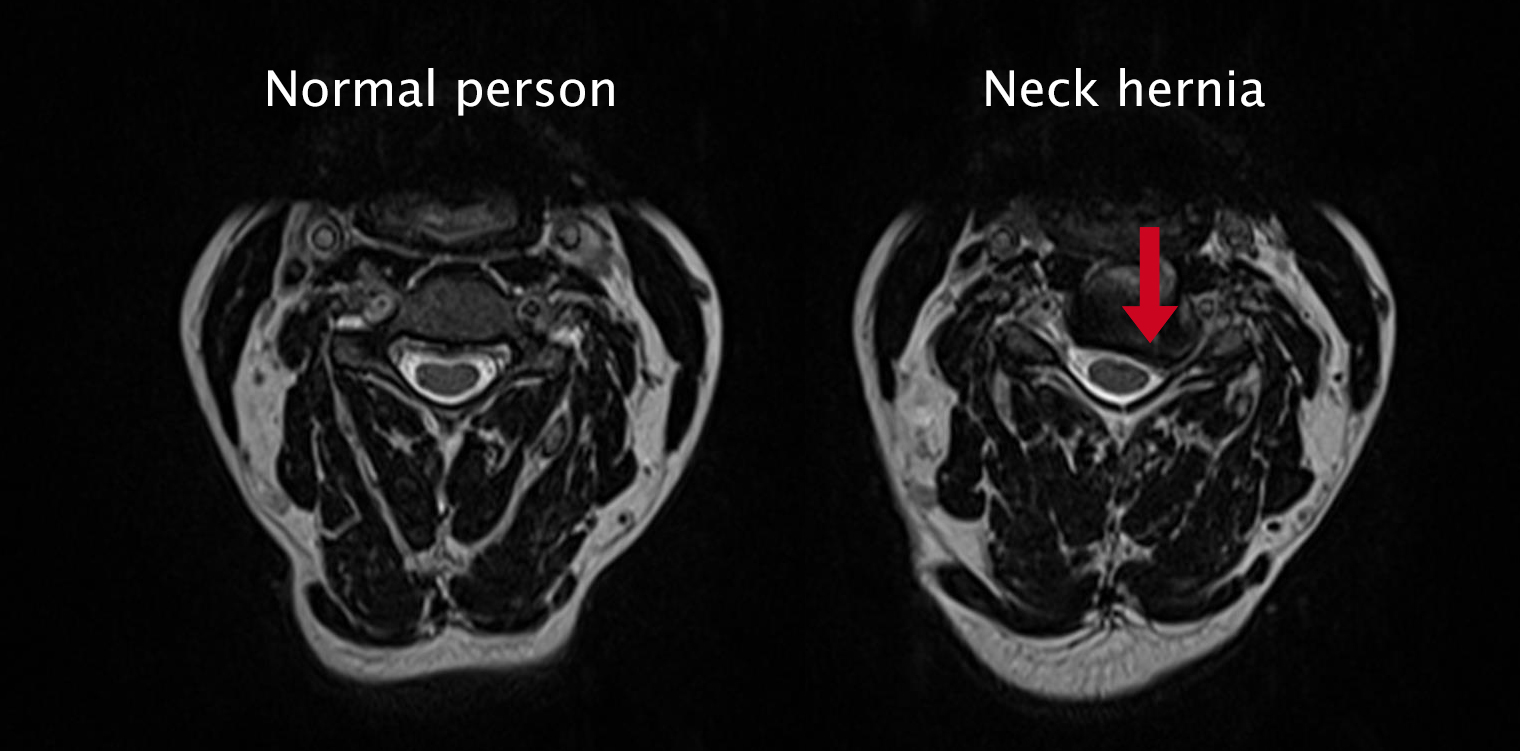
Diagnosis of a neck hernia
Additional examination
In some cases a doctor will request a CT scan of the patient’s neck, which will provide more information on the patient’s bone structure than a regular X-ray image can provide. Such an additional examination will sometimes be performed to show the size of the nerve canals in the event of a suspected bony stenosis of one of the arm nerves. Neck hernias will often present alongside stenosis of the arm nerve canal.
Surgery of a neck hernia
Not every hernia requires surgery
The neurologist will discuss with you several treatment options, whose nature will depend on the severity of your symptoms and on the neurologist’s findings after the neurological examination. Not every hernia requires surgery. Seventy to eighty percent of all hernias heal of their own accord if you just wait and rest.
Therefore, patients must not rush into surgery. On the other hand, the recovery process may take longer if a patient waits too long before undergoing surgery. Generally speaking, surgeons will wait at least six weeks before operating on a patient (unless there is an indication for emergency surgery), but will want to operate within 6 months of the onset of the pain (if the pain lasts that long).
Indications for surgery
There are two types of indications for surgery:
- Absolute: When a nerve is so severely dysfunctional that it causes paralysis or similar such symptoms. If any pressure is being exerted on the spinal cord, surgery is advisable, too.
- Relative: When an arm is so painful that it is becoming dysfunctional. Since the patient’s complaints are decisive here, it is up to the patient to decide whether or not surgery is required.
Operating on a patient from the front
At our clinics, neck hernias are generally operated on from the front, as is customary. A small incision is made at the right-hand side of the neck, through which the front of the cervical spine can easily be accessed. The operation involves pushing the trachea and oesophagus a little to the side. It does not matter which is the affected arm, since both sides of the intervertebral disc can be accessed from this point. Once the affected intervertebral disc has been removed and the outgoing nerves have been put to the side, the disc space, which is now empty, can be filled.
This can be done in various ways, using various materials. At our clinics, the empty space is filled with a plastic fusion cage that is filled with some kind of cement. This will keep the adjacent vertebrae properly aligned and the nerve canals on each side nice and open. In about a year’s time, the two vertebrae and the cage will grow into a single bone, what with the two vertebrae having fused through the cage. Once the cage has been installed, there will be no need for an additional plate on top of it. The cage will be locked into position and will not move from there.

Titanium cage
So what happens when I undergo surgery?
Click the button below for some general information on operations performed by Dr Schröder.
Risks of neck hernia surgery
Potential intra-operative risks
Like any other operation, neck hernia operations carry certain risks. However, complications are highly unlikely to occur. After all, neck hernia operations are carried out many times a year at our clinics.
In rare cases, a nerve serving the patient’s voice box may be damaged, which may cause the patient’s voice to be hoarse, either temporarily or permanently. Inflammation, haemorrhaging or subsequent bleeding may occur, as well, but these complications are likewise very rare. In addition, the sac holding the cerebrospinal fluid may spring a slight leak. This is completely harmless, although the tear must be sealed during the procedure to stop it from continuing to leak. A sealed sac always heals and patients hardly ever notice it tore in the first place. This complication, too, is highly unlikely to occur.
Since the arm nerve in the spinal canal is literally being released during the operation, there is a (very limited) chance that the person performing the surgery will cause even more damage to the nerve, which means the patient may have more pain after the operation than before. Generally, such additional symptoms will subside after a while, but in very rare cases, a little residual damage may remain. Unfortunately, this cannot be completely prevented from happening.
An even more rare complication that has been reported in the past is damage to the oesophagus. This is a severe complication requiring immediate follow-up. Since the spinal cord is located right next to the neck hernia, the spinal cord may sustain damage during the procedure. However, chances of this happening are negligible.
Hernia recurrence
Generally speaking, 8 to 9 out of 10 patients are satisfied with the results of their neck hernia surgery. Neck hernias never recur in the same spot and on the same side of the spine, as the entire affected intervertebral disc is removed during this procedure.
New hernias may occur in other parts of the spine. It is said that the adjacent vertebrae and discs carry a heavier load following the operation, which may promote the onset of problems in these adjacent body parts. However, in actual fact, this hardly ever occurs.
What is fairly common is patients experiencing both neck and spinal hernias, as the same degenerative process is at work in both the neck and the spine. After the operation, the pain radiating down the arm will be much less intense or gone completely. However, patients will experience tingling or numbness in one arm or hand following the operation. This will generally subside in the year following the operation, but may linger in some people. The neck pain, too, may persist after the operation, and may actually get worse for a for a little while. After all, a part of your spine just underwent surgery, and the wound in your neck is still ‘fresh’.
After surgery of a neck hernia
Listen to your body
Once the operation has been completed, the patient will be taken to the recovery room. Generally, s/he will have some difficulty swallowing, and his or her voice may be slightly hoarse, which will generally pass within a few days. The patient will be allowed to get up the next day, and in many cases, s/he will be allowed to go home. There is no real follow-up treatment to speak of; for instance, patients will not be required to wear a neck collar. Taking it easy for two to three weeks will suffice. After two or three weeks, the patient will be allowed to gradually resume his or her normal activities. At the follow-up appointment two weeks after the operation, we will determine whether the patient requires physiotherapy.
Our recommendation is always to listen to your body and stop doing what you’re doing when your body tells you it doesn’t like what you’re doing.






